It's Medical Monday!
- anirudhakarla
- 20 hours ago
- 3 min read
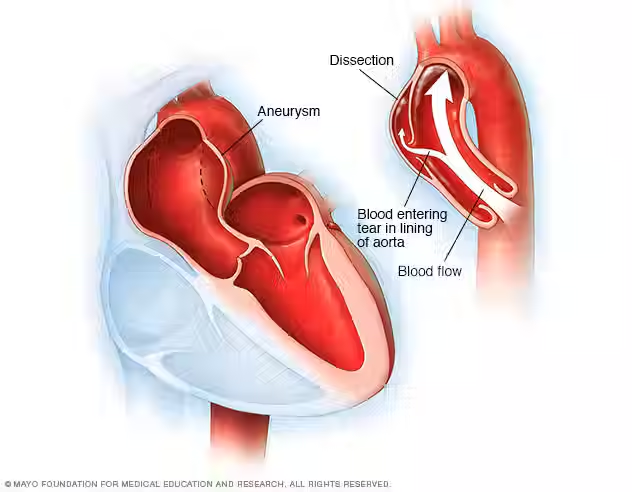
Welcome back, everyone! Today we'll be discussing one of the most serious emergencies in cardiovascular medicine, a Type A aortic dissection (TAAD). It happens suddenly, progresses quickly, and requires immediate treatment, usually emergency surgery. While the diagnosis can sound overwhelming, understanding what the condition is and why it’s so dangerous can help patients and families make sense of the urgency.
What is a Type A dissection?
As we discussed in last week's posts, the aorta is the body’s largest artery, carrying blood from the heart to the rest of the body. A dissection occurs when a tear develops in the inner lining of the aorta, allowing blood to split the layers of the vessel wall apart.
A Type A dissection involves the ascending aorta, the section closest to the heart. This is one of the most dangerous locations because several critical blood vessels branch off here to supply the heart, brain, and upper body.
Why is a TAAD so dangerous?
The ascending aorta is like a major highway intersection for blood flow. When a dissection occurs in this area, it can suddenly block or reduce blood flow to vital organs.
Some of the most serious complications include:
Stroke: The arteries supplying the brain branch off the aortic arch. If the dissection disrupts blood flow there, a stroke can occur.
Upper limb ischemia: Blood flow to the arms may become compromised, leading to pain, weakness, or loss of circulation.
Coronary malperfusion: The coronary arteries, which feed the heart itself, originate from the ascending aorta. If the dissection blocks these arteries, it can trigger a heart attack or severe heart dysfunction.
Aortic rupture: The weakened vessel wall can tear completely, causing life-threatening internal bleeding in the chest.
Aortic valve failure: The dissection can affect the aortic valve, leading to severe leakage and sudden heart failure.
Because these complications can happen very quickly and often require immediate care, Type A dissections are treated as immediate surgical emergencies.
What symptoms can occur?
The classic symptom is sudden, severe chest pain, often described as tearing or ripping. The pain may begin or move into the back, neck, or abdomen.
Other symptoms can include:
Fainting
Shortness of breath
Weakness or numbness
Trouble speaking
Loss of pulse in an arm
Symptoms vary depending on which blood vessels are affected.
How do you fix it, and what happens afterwards?
During surgery, the patient is put on cardiopulmonary bypass, and the damaged portion of the aorta is replaced with a synthetic graft. Depending on the situation, surgeons may also repair the aortic valve or address affected coronary arteries. The goal is simple but critical: restore normal blood flow and prevent rupture.
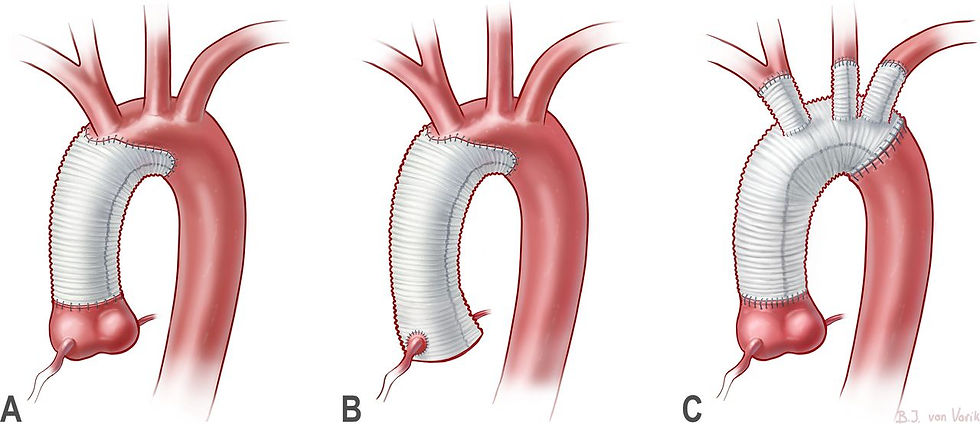
Recovery can take time, but many patients go on to live active, meaningful lives after surgery. Long-term care typically includes:
Strict blood pressure control
Regular CT scans or echocardiograms
Lifelong follow-up with cardiovascular specialists
Ongoing monitoring is important because the remaining portions of the aorta still need careful observation over time.
Bottom line
A Type A aortic dissection is a true surgical emergency because it affects the part of the aorta responsible for supplying blood to the heart, brain, and upper body. Without rapid treatment, complications such as stroke, heart attack, or rupture can become fatal very quickly.
Fast diagnosis and emergency surgery save lives. Understanding the condition can help patients and families navigate an incredibly stressful situation with a little more clarity.
'Till next time,
Anirudh Karla



Comments