It’s Medical Monday!
- anirudhakarla
- Apr 13
- 2 min read
Welcome back, everyone! After talking about thoracic aortic aneurysms last week, today we’ll be discussing abdominal aortic aneurysms. An abdominal aortic aneurysm, often called an AAA, is a condition that many people have never heard of, yet it can be serious if left untreated. The good news is that when it’s found early and monitored properly, it can often be managed safely.
Here’s a simple breakdown of what an AAA is and what it means for your health.
What is an abdominal aortic aneurysm?
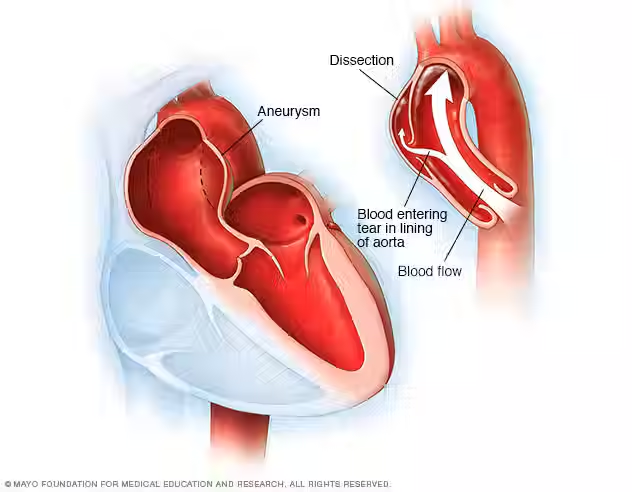
The aorta is the largest artery in your body, running from your heart down through your chest and abdomen. An abdominal aortic aneurysm occurs when a section of the aorta in the abdomen becomes weakened and bulges outward, like a balloon.
Over time, that bulge can grow larger. If it becomes too large, there’s a risk it could rupture, which is a medical emergency.

Who is at risk?
AAAs are more common in certain groups of people, including:
Adults over age 65
People with a history of smoking
Those with high blood pressure
Individuals with a family history of aneurysms
Many people with an AAA don’t have symptoms, which is why screening and imaging are so important in higher-risk groups.
Are there any symptoms?
Most abdominal aortic aneurysms are silent, meaning they don’t cause noticeable symptoms. When symptoms do occur, they may include:
A pulsating feeling in the abdomen
Deep, steady abdominal or back pain
A ruptured aneurysm can cause sudden, severe pain, dizziness, or fainting and requires immediate emergency care.
How is it diagnosed?
AAAs are often found incidentally during imaging tests done for other reasons. They can also be detected through:
Ultrasound (commonly used for screening)
CT scans or MRI for more detailed imaging
Screening is recommended for certain high-risk individuals, especially older adults with a history of smoking.
How is it treated?
Treatment depends largely on the size of the aneurysm and how quickly it’s growing.
Small AAAs: Often monitored with regular imaging and managed with blood pressure control and lifestyle changes.
Larger or growing AAAs: May require repair to prevent rupture.
There are two main types of repair:
Open surgical repair, where the weakened section is replaced with a graft
Endovascular repair (EVAR), a less invasive approach using a stent graft placed through the blood vessels
Your doctor will recommend the best option based on your anatomy and overall health.
Why monitoring matters
Even if an AAA doesn’t need immediate surgery, regular follow-up is essential. Watching for changes in size helps ensure that treatment can happen before complications develop.
Bottom line
An abdominal aortic aneurysm is a serious condition, but it’s often manageable—especially when caught early. Many people live for years with small, stable aneurysms under careful monitoring.
If you’re in a higher-risk group or have a family history, talk to your doctor about whether screening is right for you. Staying informed and keeping up with follow-up care can make all the difference.
That's all for this week, folks. Thanks for joining us again!
Till next time,
Anirudh Karla



Comments